Understanding the Causes and Prevention of Varicose Veins
December 22, 2023Demystifying Varicose Veins: Causes, Symptoms, and Complications
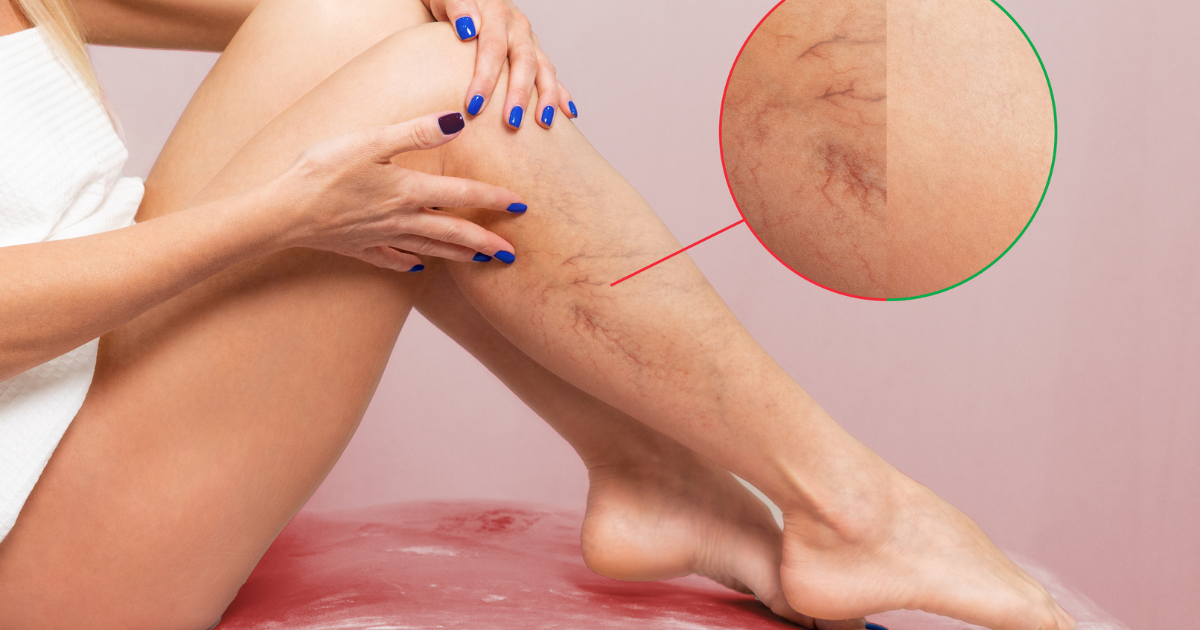
Varicose veins are a common condition characterized by enlarged, twisted veins, primarily occurring in the legs. Understanding the causes, symptoms, and potential complications associated with varicose veins is essential in promoting prevention and effective management. Varicose veins develop when the valves within the veins malfunction, leading to blood pooling and vein enlargement. The weakened or damaged valves are unable to efficiently push blood back to the heart, causing it to flow backward and accumulate in the veins.
Symptoms of varicose veins can vary from mild to severe. Common symptoms include pain, aching, throbbing, heaviness, and swelling in the legs. The affected veins may appear dark blue or purple and may be visible through the skin. In some cases, varicose veins can cause complications such as venous ulcers, skin discoloration, blood clots, and superficial thrombophlebitis.
Risk Factors That Increase the Likelihood of Developing Varicose Veins
Understanding the risk factors that lead to the development of varicose veins can help people assess their own risk and take proactive steps to control or avoid the condition. Given that the natural aging process wears down the veins’ walls and valves, advanced age is a substantial risk factor for varicose veins. Vein hypertrophy and valve malfunction are more likely to occur as people age because the veins lose some of their strength and suppleness.
The development of varicose veins is also influenced by gender, with women being more prone to the ailment than males. Women are more at risk due to hormonal changes brought on by puberty, pregnancy, and menopause. The body produces more estrogen and progesterone during pregnancy, which can soften vein walls and impede valve performance. Additionally, the expanding uterus may put pressure on the pelvic veins, obstructing blood flow and raising the possibility of developing varicose veins in the legs.
Genetics and family history have a significant impact on varicose vein susceptibility. If you have a parent or sibling with varicose veins, you are more likely to develop the condition yourself. Genetic factors influence the structure and integrity of vein walls and valves, making them more prone to malfunction. While you cannot change your genetic makeup, being aware of your family history can prompt early intervention and preventive measures.
Lifestyle factors also contribute to varicose vein formation. Jobs that involve prolonged periods of standing or sitting can increase the risk. Standing for long hours without breaks or engaging in activities that require extended periods of sitting, such as desk jobs, can hinder proper blood circulation and lead to the development of varicose veins. Occupations that involve heavy lifting or straining can also contribute to the condition.
Obesity and a sedentary lifestyle are additional risk factors for varicose veins. Excess weight puts added pressure on the veins, impeding blood flow and leading to valve dysfunction. Lack of physical activity further compounds the problem by limiting muscle contractions that help propel blood upward against gravity. Regular exercise, on the other hand, promotes blood circulation, strengthens the leg muscles, and reduces the risk of varicose veins.
A history of blood clots, damage to the veins, and illnesses that raise intraabdominal pressure, such as persistent constipation or liver disease, are additional risk factors. Due to their effects on vein flexibility and blood clotting, hormonal medications like hormone replacement therapy or birth control tablets can also raise the risk of varicose veins.
Identifying people who are more prone to varicose veins requires an understanding of these risk factors. Individuals can adopt preventative steps and proactive efforts to lower their risk by being aware of these factors. Varicose veins can be prevented by engaging in regular exercise, eating a balanced diet, avoiding extended standing or sitting, and adopting other healthy lifestyle practices. A healthcare expert should be consulted if you have certain risk factors or worries so they can provide you with individualized advice and direction.
The Link Between Genetics and Varicose Vein Development
Understanding the connection between genetics and this ailment can offer helpful insights into its prevention and management. Varicose vein development has a substantial hereditary component. You are more prone to get varicose veins if your family has a history of having them. Inherited features that have an impact on vein anatomy, valve function, and general vein health are the cause of the genetic influence on varicose veins.
Research has shown that certain genetic factors contribute to the weakening of vein walls and valves, making them more susceptible to dysfunction. These genetic variations can impact the production and structure of collagen and elastin, proteins that play a vital role in maintaining the integrity and elasticity of veins. Changes in these proteins can lead to decreased vein strength and flexibility, increasing the risk of varicose veins.
Additionally, research have discovered particular gene variations linked to varicose veins. Variations in the extracellular matrix component-related genes COL4A1, COL14A1, and COL15A1 have been associated with an increased risk of developing varicose veins. These genes play a role in the development and upkeep of connective tissues, including vein connective tissues.
Twin and family studies provide more evidence that genetics have a role in varicose vein development. According to these research, identical twins had a greater concordance rate for varicose veins than fraternal twins, which points to a significant genetic component. Varicose veins are more common among first-degree relatives of those who have them, according to family research.
While genetics plays a significant role, it is important to note that varicose veins can also be influenced by environmental and lifestyle factors. For example, hormonal changes during pregnancy or the use of hormone therapies can exacerbate the condition, even in individuals with a genetic predisposition. Similarly, obesity, lack of physical activity, and prolonged periods of sitting or standing can contribute to varicose vein development, regardless of genetic factors.
Understanding the genetic link to varicose veins provides an opportunity for early intervention and preventive strategies. Individuals with a family history of varicose veins should be aware of their increased risk and take proactive measures to minimize its impact. While genetics cannot be changed, lifestyle modifications such as regular exercise, maintaining a healthy weight, avoiding prolonged sitting or standing positions, and wearing compression stockings can help reduce the likelihood of varicose vein development.
Additionally, individuals with a strong genetic predisposition may consider regular check-ups with a healthcare professional specializing in vein health. This proactive approach allows for early detection, intervention, and personalized management strategies to minimize symptoms and complications associated with varicose veins.
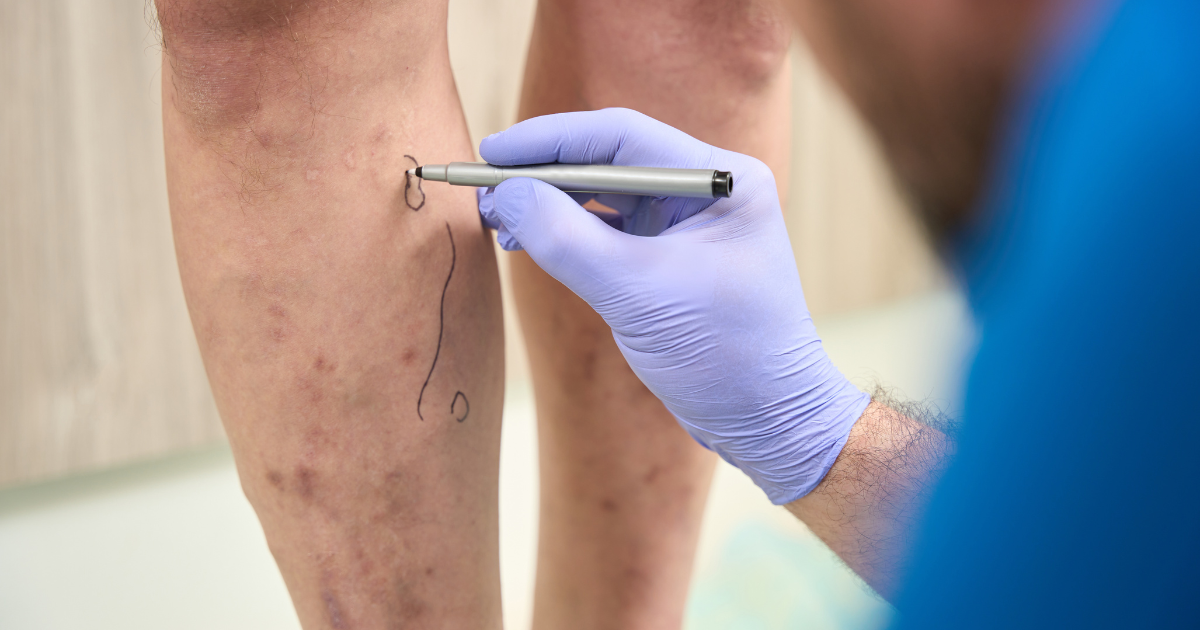
The Impact of Lifestyle Choices on Varicose Vein Formation
Lifestyle choices significantly contribute to the development of varicose veins. Prolonged periods of standing or sitting can hinder proper blood circulation and increase the risk of vein dysfunction. Occupations that involve prolonged standing, such as nursing or retail, and occupations that require extended periods of sitting, such as desk jobs, can both contribute to varicose vein formation. Regular movement and avoiding immobility for long periods are crucial in preventing vein-related issues.
Exercise and Physical Activity for Varicose Vein Prevention
Engaging in regular exercise and physical activity is a powerful preventive measure against varicose veins. Physical movement helps promote healthy blood circulation, strengthens the leg muscles, and improves overall cardiovascular health. Activities such as walking, swimming, cycling, and low-impact exercises can be beneficial in preventing varicose veins.
Maintaining a Healthy Weight to Reduce Varicose Vein Risk
In order to lower the risk of varicose veins, it is crucial to maintain a healthy weight. Being overweight puts more strain on the veins, which reduces blood flow and raises the risk of vein dysfunction. People may reach and maintain a healthy weight by eating a balanced diet and exercising often, which will ease the strain on their veins and improve their vein health in general.
Strategies for Improving Blood Circulation to Prevent Varicose Veins
Improving blood circulation is crucial in preventing varicose veins. Simple strategies such as elevating the legs, avoiding tight clothing that restricts blood flow, and taking regular breaks to move around can help enhance circulation. Additionally, avoiding exposure to excessive heat, such as hot baths or saunas, can prevent vein dilation and promote healthy blood flow.
Avoiding Prolonged Sitting and Standing Positions
Prolonged sitting or standing can adversely affect blood circulation and increase the risk of varicose veins. Individuals in occupations that involve prolonged sitting should make an effort to take regular breaks and incorporate movements into their routine. Similarly, those with jobs that require prolonged standing should find opportunities to rest and elevate their legs periodically to improve blood flow.
Tips for Choosing Suitable Footwear to Support Vein Health
Choosing appropriate footwear is an often overlooked aspect of varicose vein prevention. Opting for shoes that provide proper support and cushioning can help improve blood circulation and reduce the risk of vein-related problems. Avoiding high heels and tight-fitting shoes that restrict foot movement is advisable. Instead, opt for comfortable, low-heeled shoes that allow for natural foot movement.
How to Incorporate Dietary Changes to Support Vein Health
While diet alone cannot prevent or cure varicose veins, certain dietary changes can support vein health and overall circulation. Incorporating foods rich in fiber, such as fruits, vegetables, whole grains, and legumes, can prevent constipation and promote healthy blood flow. Staying adequately hydrated by drinking plenty of water is also important for maintaining optimal circulation and preventing vein-related issues.
In conclusion, understanding the causes and prevention of varicose veins is vital for maintaining healthy veins and reducing the risk of complications. People can prevent varicose veins and advance vein health by being aware of the risk factors, living a healthy lifestyle, exercising frequently, keeping a healthy weight, enhancing blood circulation, and making educated dietary decisions.
What to do if you already have varicose veins?
When it comes to varicose veins treatmnet, surgical interventions are often considered in cases where conservative measures have not provided sufficient relief or when the varicose veins are severe. Surgical solutions aim to remove or close off the affected veins, redirecting blood flow to healthier veins. Vein ligation and stripping, ambulatory phlebectomy, endovenous ablation techniques (such as laser or radiofrequency ablation), and foam sclerotherapy are among the surgical options available.
Vein ligation and stripping involve making small incisions near the affected veins, tying them off, and removing them through the incisions. This procedure can effectively alleviate symptoms and improve the cosmetic appearance of varicose veins. Ambulatory phlebectomy, a minimally invasive procedure, allows for the removal of the affected veins through small incisions. These procedures are typically performed on an outpatient basis, and patients can expect a gradual return to their normal activities within a few weeks.
Endovenous ablation techniques, such as laser or radiofrequency ablation, are used to close off the affected veins. During these procedures, a thin catheter is inserted into the vein, and either laser energy or radiofrequency waves are used to heat the vein, causing it to seal shut. This redirects blood flow to healthier veins, improving symptoms and reducing the appearance of varicose veins. Foam sclerotherapy involves injecting a special foam solution into the affected veins, causing them to collapse and eventually be absorbed by the body.
Surgical treatment for varicose veins should be performed by qualified healthcare professionals, typically vascular surgeons or interventional radiologists, in appropriate clinical settings. Dr. Ahmed Farah Abdulrahman is the perfect choice if you reside in Dubai! He has the expertise and experience to determine the most suitable surgical options based on the individual’s specific condition and medical history.
It is crucial to remember that, similar to any surgical procedure, varicose vein surgery carries certain risks and potential complications, including infection, bleeding, scarring, and nerve damage. However, with advancements in surgical techniques and technologies, these risks are generally low when performed by experienced surgeons such as Dr. Farah.
After surgical treatment, patients are often advised to wear compression stockings to aid in healing, reduce swelling, and promote optimal blood circulation. Following post-operative care instructions provided by the healthcare professional is essential for proper recovery.
In conclusion, surgical interventions play a significant role in the treatment of severe varicose veins. Procedures such as vein ligation and stripping, ambulatory phlebectomy, endovenous ablation techniques, and foam sclerotherapy can effectively alleviate symptoms and improve vein health. It is important for individuals considering surgical treatment to consult with a qualified healthcare professional specializing in vein disorders to determine the most appropriate procedure based on their specific condition. With proper evaluation and skilled surgical intervention, individuals with severe varicose veins can experience symptom relief and an improved quality of life.
